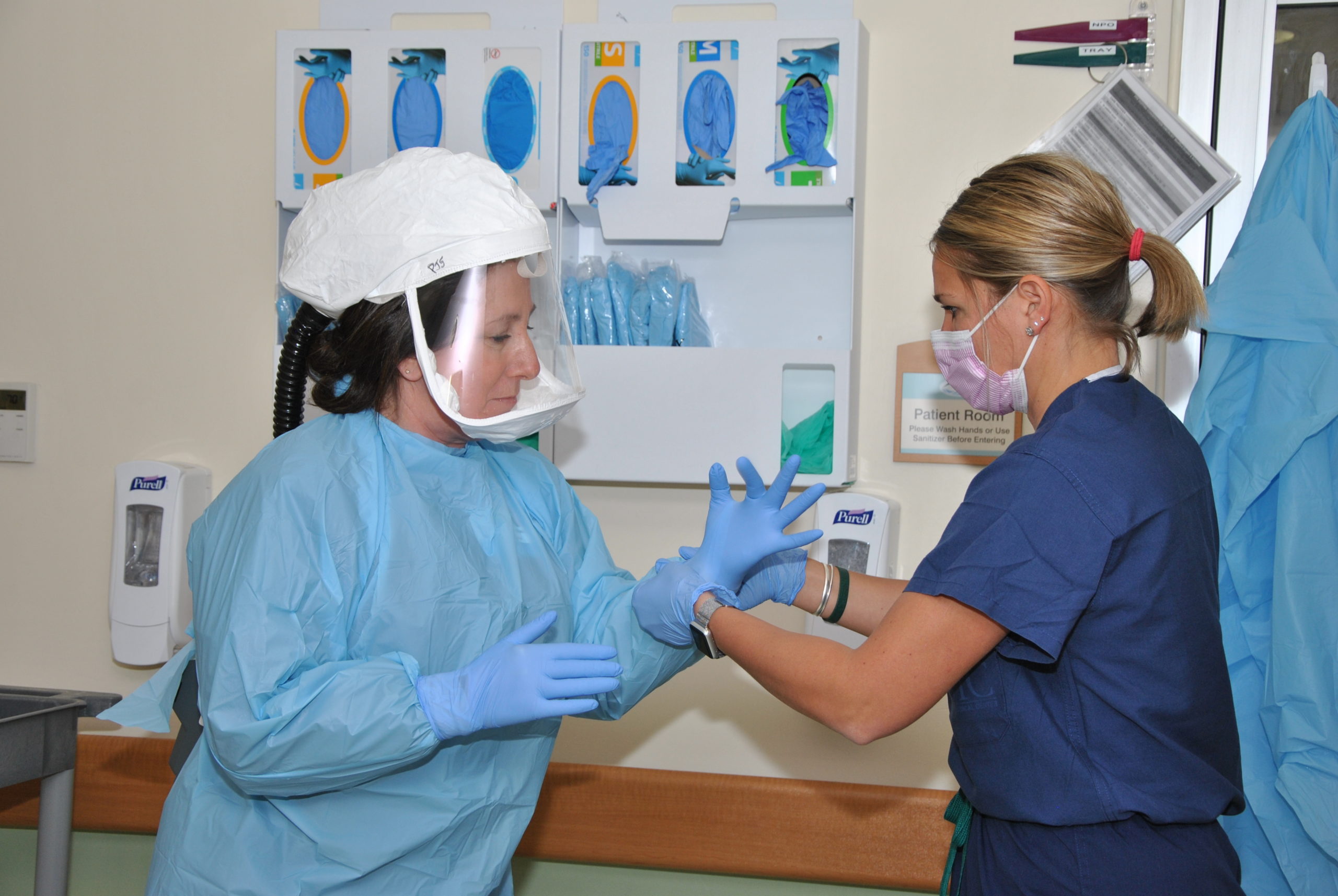

Life Behind the Mask: Innovative Observer System Prevented Infections
When the reality of the COVID-19 pandemic set in, a key part of NMC’s preparations revolved around safety: the safety of patients, family, the public … and the safety of hospital staff. It was critical that staff safety was of highest priority, for without them, we could not care for our patients.
One of the concrete outcomes of the intense safety discussions was the creation of a new clinical role – that of a Personal Protective Equipment (PPE) “observer” who oversees nurses and providers when they enter patient rooms, instructing them in how and when to put on and take of gowns, gloves, hair coverings and masks. It sounds like a simple change, but it’s one that had enormous impact.
The Worries about Infection and Cross-Infection
“We are all aware of how many healthcare workers had become infected with COVID-19 in other areas,” said Anneke Merrit, NMC’s Director of Quality. “This role was critical in protecting our staff. It was also critical in preventing spread of COVID-19 from positive patients to COVID-19 negative patients.”
According to a Reuters report with data from the International Council of Nurses, at least 90,000 health-care workers worldwide are believed to have been infected with COVID-19.
Courtney Leduc, a former Emergency Department nurse who now works in Pediatrics at NMC said the idea for an observation process came from Emergency Preparedness training she and other NMC’ers attended in Alabama. “Close observation will save your healthcare workers,” she recalls hearing and those words floated through her mind as she met with other NMC staff who were trying to prepare in the early stages of the pandemic.
Nearly overnight, Leduc and “the PPE team” as they came to be known, devised a protocol for the observations, requiring strict adherence to precisely directed verbal instructions. Watching an observer-caregiver pair in action is awe-inspiring. Every single step is orchestrated and called out by the observer, who tells the care-giver exactly when to sanitize their gloves, remove their outer gloves, sanitize again, remove headcoverings, remove and clean the clear face-shield, remove the gown, hang the gown, sanitize again and so on.
The methodical, step-by-step process is important. Wearing PPE is physical uncomfortable, exhausting and sweaty. Working in those conditions in close quarters with sick patients who may or may not have a high-consequence infectious disease can produce high anxiety and deep emotions. When a provider is ready to take off PPE (a process called doffing), the tendency is to want to get it off as quickly as possible. The PPE observer helps control that process and ensure the steps are done properly.
“Staff come out of rooms soaking wet, physically exhausted, emotionally fried,” said Leduc. “You’re their nurse and now you’re also their family members,” she said, referring to the absence of visitation from family during the pandemic.
Finding a Way at a Feverish Pace
Figuring out how to do this, do it safely, and find a team to take shifts in the role was a big job. The effort was led by NMC’s Quality Department, which quickly tapped into the Emergency Department and Surgical Services nurses as the highly-skilled staff who jumped in to help in unprecedented ways.
“I was inspired by the professionalism, ownership and accountability to provide excellence in keeping one and other safe,” said Chief Nursing Officer Deanna Orfanidis, RN. “This process allowed the staff the opportunity to focus on the care of the patient knowing someone had their back in this high-risk situation.”
The new role meant that NMC needed to find additional nurses to cover all shifts in a 24/7 environment. Despite the need for more staff, despite the unknowns, despite daycare dilemmas and grocery shortages – NMC’ers stepped up.
“There is a reason people are in healthcare and this kind of thing proves why,” said Leduc of the incredible dedication shown by staff during the care of COVID patients.
“I have been humbled and honored to be part of such a high functioning team with unwavering commitment to patients and one and other,” said Orfanidis.
The design and implementation of this role occurred incredibly rapidly. Leduc said it was around-the-clock work that needed to be done almost overnight, preparing for the inevitable first patient.
“It’s been a wild ride of very charged emotions,” she said.
One Team, United for Safety
A hallmark of all NMC’s COVID-19 response efforts was the way staff from different departments pitched in at a moment’s notice, often taking on new roles like that of the PPE observer.
“It’s been such a pleasure working with this team. I enjoyed getting to know the Surgical Services nurses, and strengthening relationships with the nurses I had worked with in the past,” said Merritt.
Samantha Owen is one of the Emergency Department nurses who benefited from the PPE observer role and said she was a welcome addition during a stressful time. She said that most of her anxiety in working with COVID patients came from the near-constant change of protocols. “We had to learn on the fly and be very accepting of change. The PPE observer helped with the policy changes and kept us updated.”
Owen also said that having someone care for the care-givers was very welcome. The air flow machines in COVID-19 negative pressure rooms are noisy and elderly patients who couldn’t hear well had even higher levels of anxiety, leading Sam to spend time sitting with them, gowned in full PPE, simply to have someone nearby.
All while an observer kept watch from outside, kept track of time, kept track of PPE stock, kept spaces clean … and pulled her out when a break was necessary. As of today, NMC has experienced no COVID-19 infections of staff from contact with patients, and also seen no patient-to-patient infections – a remarkable achievement.
It was a much-needed innovation that NMC will keep in place, to be used as needed for any patient requiring isolation. It remains a testament to compassionate caring and professionalism. “I was incredibly impressed and proud,” said Merritt. “I hope they are proud of the work they have done.”
